As you can tell from the opening, I originally posted this on my Substack in October. Inspired by Jason Crawford's post on curing cancer, I'm reposting it here. I will note that Her2+ breast cancer was not the first once-fatal disease with which I had a scrape. As a child, around 1967, I had scarlet fever, which before antibiotics could kill, as readers of Little Women know.

I think about breast cancer every October, and not because it’s “Breast Cancer Awareness Month,” which I find some mixture of ridiculous and distasteful. I’m all for raising money for breast cancer research and treatment. But making people “aware” by slapping pink on everything from the water in public fountains to specials at Dollar Tree doesn’t do much to save lives. When someone’s selling “breast cancer awareness” tchotchkes, any contributions won’t be more than their profit margins and quite likely less. (See this 2015 Business Insider analysis of how little money from the NFL’s breast cancer merch makes it to the cause.)
It’s not the orgy of pink that reminds me of breast cancer. It’s the Nobel Prize in Physiology or Medicine. I have a rooting interest, and so far I’ve been disappointed. I want the prize to go to UCLA cancer researcher Dennis Slamon, who in recent years has been on the Great Mentioner’s short list (an improvement since I started paying attention a decade or so ago).
Slamon’s work did two things: Beginning with HER2+ breast cancer, it demonstrated that cancers could be identified by specific genetic variants, rather than merely where they occur in the body. Then it showed that those variations could be targeted and treated with specific antibodies. The first practical result was the drug Herceptin, which treats the roughly 25 percent of breast cancer patients with an especially aggressive form. From a recent UCLA profile:
The key finding by Dr. Slamon and colleagues showed that the monoclonal antibody Herceptin binds to, and destroys, abnormal cells without harming nearby healthy tissue, much like a laser-guided missile hitting a select target. This was a major departure from then-common chemotherapies that Dr. Slamon refers to as the “hand grenade” approach, indiscriminately killing healthy as well as diseased cells. Proving that antibodies that bind to cancerous cells are an effective method for treating solid tumors transformed cancer care at a time, in the 1980s, when most cancer therapies were focused on excising tumors and developing better chemotherapies. The discovery opened up new research avenues, leading to multiple other targeted treatments that utilize antibodies to attack the disease at its genetic roots. Between 2.7 million and 3 million women have been treated with Herceptin, and women with HER2-positive breast cancer now have among the highest survival rates compared with all women with breast cancer.
Here’s a video that explains further (and includes researchers Axel Ullrich and H. Michael Shepard, who might share in the same prize, as they did in the Lasker award sometimes called the “American Nobel”1).
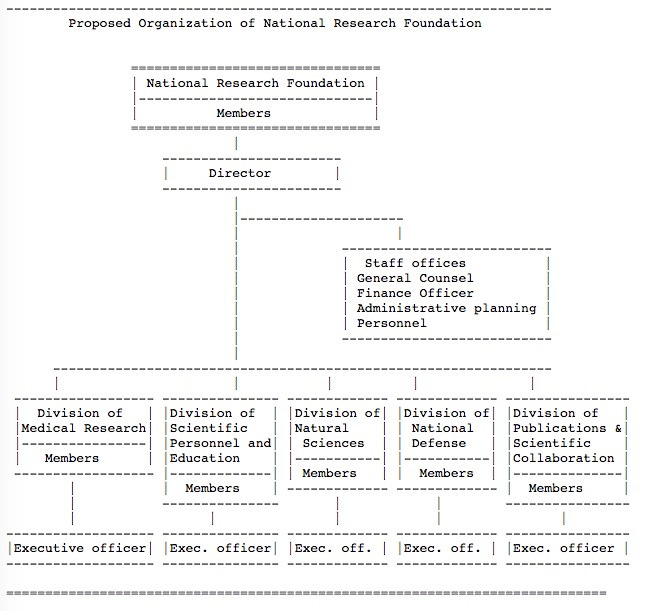
If U.S. scientific research were more “efficiently” funded, none of this research might have happened. After the scientific triumphs of World War II, Vannevar Bush, who had directed the wartime Office of Scientific Research and Development, proposed the establishment of a similar peacetime organization through which all science funding would flow. After some legislative iterations, we got the National Science Foundation, but it has no monopoly even on federal government funding. In addition to the obvious National Institutes of Health, money flows from assorted pockets of the Defense Department, the Energy Department, and more. On top of that are many philanthropic foundations, including heavy hitters like the Howard Hughes Medical Institute, the Bill & Melinda Gates Foundation, and the American Cancer Society. To a good technocrat like Bush, it would seem like a disorganized mess.
Back in the 1980s, Slamon amassed a collection of different kinds of cancer tumors removed from patients, believing that analyzing their cells’ molecular biology could unlock the mystery of why the cancers spread. UCLA wasn’t a major cancer-research institution, Slamon was a nobody, and his idea was decidedly out of the mainstream. You can imagine how his grant proposals were received. When he applied for an NIH grant to fund the tumor bank, he says, “It came back with a laugh track.”
Fortunately Axel Ullrich, then at Genentech, gave a seminar at UCLA, presenting his work on growth-regulating genes. He agreed to give Slamon samples of the DNA he’d identify to test against the tissues in the tumors. To do the painstaking work on a low budget, Slamon hired a UCLA freshman named Wendy Levin:
Now a physician, Dr. Levin is an oncologist in San Diego County, but while an undergraduate, she spent nights and weekends “sometimes sleeping on the floor in the lab,” she says, extracting DNA from tumors. It was tedious work, taking a piece of tumor tissue that had been frozen in liquid nitrogen, grinding it up, extracting the DNA and looking at one gene at a time for something awry. But the work bore fruit on a Saturday afternoon in June of 1986, when she found a match between the HER2 gene and a breast cancer tumor. “My heart started thumping,” Dr. Levin says. “It was a true eureka moment.” She excitedly called Dr. Slamon at home, offering to drive out to his house to show him the results. Dr. Slamon decided it would be OK to wait until Monday.
The usual sources were still not interested in paying for research. But in 1989, Slamon was treating Hollywood honcho Brandon Tartikoff, best known for his stint as president of NBC, for Hodgkin’s lymphoma. Tartikoff’s wife Lilly was grateful for the care and asked Slamon what she might do to help him. He told her about the idea of finding a drug to treat HER2+ breast cancer. Soon thereafter, in a classic Hollywood moment, she ran into Ronald O. Perelman, who owned Revlon, at Wolfgang Puck’s original Spago restaurant. She gave him the pitch: You own Revlon. Revlon sells to women. Women get breast cancer. You and Revlon should support this research. He agreed to let his representative meet with Slamon.
At the meeting, Slamon was accompanied by his colleague John Glaspy, who is a notably blunt-spoken person. Even if they got government funding, Glaspy warned, it would take several years and by then “we’ll have a Rose Bowl full of dead women” from breast cancer. The pitch worked. As Mona Gable recounted in a 1998 article for UCLA Magazine:
Perelman not only came through for Slamon, but he made an astonishing offer: $800,000 a year for three years, a total of $2.4 million. As support from an American corporation to a single scientific group, the gift was virtually unprecedented. Just as amazing, the research funding was unrestricted. Slamon could use the money however he saw fit.
“It would have taken four concurrent National Cancer Institute grants to build the equivalent of the program Revlon funded with just the stroke of a pen,” Slamon says intently. “And there was no writing a grant, submitting it, waiting eight to 12 months to hear. This gift allowed us to follow our leads almost instantaneously, and made a huge difference in this whole story.”
Even with Revlon’s help—and money from one of those Pentagon pockets—the development of Herceptin was such a difficult journey that it became a Lifetime movie. Genentech was a young company with little margin for error and several times threatened to cancel drug development.
In 1998, the drug was approved for treatment of Stage 4 HER2+ breast cancer and in 2006 it was approved for treating early stage cancers. A year later, it saved my life. As I wrote in the acknowledgements in The Power of Glamour:
In July 2007, barely a week after receiving the final signed contract for the book, I was diagnosed with what turned out to be HER2-positive breast cancer, a particularly aggressive form of the disease. Twenty years earlier, I would have had only a fifty-fifty chance of survival, given the details of my case. Today, I am officially cured. Although I underwent the traditional treatments of surgery, chemotherapy, and radiation, what made the crucial difference was the pathbreaking biologic drug Herceptin, first approved by the Food and Drug Administration in 1998.
The research that led to Herceptin was funded not by the federal government or a traditional cancer charity but by money from Ronald O. Perelman, in his role as chairman of Revlon, and by fundraising in the 1990s at a series of star-studded events called the Fire and Ice Balls. I am deeply grateful to the many people, only one of whom I know personally, responsible for bringing Herceptin to the world: to Dennis Slamon for his scientific vision; Lilly Tartikoff for her fund-raising energy; my oncologist, John Glaspy, for his persuasive eloquence; the researchers at Genentech for development and testing; and Perelman and Revlon for their financial contributions. In a very real way, I owe my life to the glamour of makeup and movie stars.
As the ever-frank Dr. Glaspy told me, “You’re cured, and if you ever get breast cancer again, it won’t be the same cancer.”

1 Analogous, minus the age restrictions, to the John Bates Clark Award in economics as a predictor of future Nobelists.

Amazing story, and fantastic post, thanks!